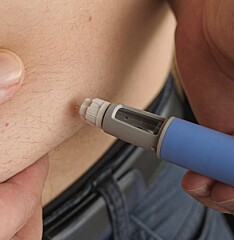
Experts are changing their views on the treatment of obesity in children
Aggressive treatment with medication and surgery is now being recommended in the United States if lifestyle changes do not produce results. Norwegian experts have also changed their views in line with this.
Overweight and obesity affect millions of young people worldwide. In Norway, 15 to 21 per cent of all children and young people are overweight. Around three per cent fall in the obesity category.
In the United States, almost 20 per cent of all children and adolescents suffer from obesity.
This poses a significant health problem. When you have obesity in childhood, the risk is high that the disease will follow you into adulthood. Obesity is in turn linked to a number of other health problems, such as diabetes, heart disease and depression.
Standard treatment for children with obesity is lifestyle treatment – which requires changing dietary and exercise habits. However, a great deal of research shows that this approach is not very effective for the vast majority of people.
Nevertheless, the attitude has long been to wait and see, writes the Associated Press News (AP) in the USA. Healthcare professionals have been cautious about invasive measures and have chosen instead to see if youngsters outgrow obesity.
But attitudes toward this are changing, in Norway as well as in the US. The American Academy of Pediatrics (AAP) is doing a U-turn.
Medication and surgery recommended
“Waiting doesn’t work,” Ihuoma Eneli tells AP.
She is one of a number of researchers behind the organisation's new guidelines for the treatment of obesity in children and adolescents.
The researchers believe that the previous attitude has only led to further weight gain and a greater risk of obesity in adulthood.
Now the AAP recommends following up with more aggressive treatment when lifestyle treatment is not enough, including offering weight-reducing drugs to children over age 12 and surgery to adolescents over age 13.
It'as probably no coincidence that these pieces of advice are coming now.
Recent years have seen a major development in anti-obesity medications. A 2022 study showed that the substance semaglutide, under the product name Wegovy, worked very well to treat obesity in adolescents.
Diet and exercise alone not useful for many
The attitude among professionals has been evolving alongside the obesity medications. The new guidelines aim to correct a mistaken perception that obesity is a personal problem that is primarily about lifestyle choices, AP writes.
The guidelines refer to obesity as a complex, chronic disease which is largely due to biological factors, rather than a lack of character and willpower.
“I definitely think this is an acknowledgment that diet and exercise aren’t helpful for many teenagers who struggle with this disease – perhaps even the majority of them,” Stephanie Byrne, a paediatrician at Cedars Sinai Medical Center, tells the AP.
Byrne has not been involved in designing the new guidelines, but agrees with the updated focus on rapid and intensive treatment. At the same time, Byrne believes that we need more research into the long-term effects of the anti-obesity drugs.
Similar change in Norway
“The attitude towards active treatment is also changing in Norway,” says Jøran Hjelmesæth. He is a professor at the University of Oslo and heads the Morbid Obesity Centre (MOC), Health Region South-East in Vestfold.
He and colleagues from obesity clinics throughout the country recently wrote an article about the topic, published in The Norwegian Medical Association journal Tidsskriftet (link in Norwegian).

The researchers write that they are still cautious about recommending weight-loss (or bariatric) surgery for adolescents. Although such operations often result in a large reduction in weight, there is also a risk of serious side effects.
But anti-obesity drugs have taken on a new role.
Over a hundred teens with severe obesity have already started taking the obesity-reducing drug liraglutide in addition to lifestyle treatment. The preliminary findings are that the treatment can yield good results in cases where lifestyle treatment alone does not work, the researchers write.
Hjelmesæth also says that a large Norwegian study of semaglutide involving several research centres is being planned. The study is scheduled to start in January 2024.
Only for the rich?
The question, however, is how easy it will be to make this offer to Norwegian youth.
In January, it became clear that the Norwegian Medicines Agency will not grant a so-called blue prescription for the drug Wegovy, which contains semaglutide. This means that the patients themselves will need to pay for the treatment, which costs NOK 36 000 a year.
Einar Andreassen, senior advisor in the Norwegian Medicines Agency, justified denying reimbursement for Wegovy, saying that the price of the medicine is not in reasonable proportion to its health effect.
“We believe that the medicine is not cost effective, that it’s too expensive in relation to documented health effects,” he said.
Recently, it was also announced that the established medicine Saxenda, with liraglutide, will be removed from the blue prescription scheme.
Hjelmesæth believes this means that obesity-reducing drugs will only be available to the rich.
This is the situation in the USA as well, according to AP. There the price is even higher than in Norway and many insurance companies probably will not cover these medications.
———
Read the Norwegian version of this article at forskning.no