Quicker treatment of newborn jaundice brings big benefits
More effective light therapy reduces the risk of brain damage and minimizes infants’ separation from parents
Denne artikkelen er over ti år gammel og kan inneholde utdatert informasjon.
One quarter of newborns admitted to neonatal intensive care receive treatment for jaundice. The risk of jaundice is especially high for preemies, and 8 out of 10 extremely premature infants require treatment. Babies can suffer brain damage if serious jaundice is not detected and promptly treated.
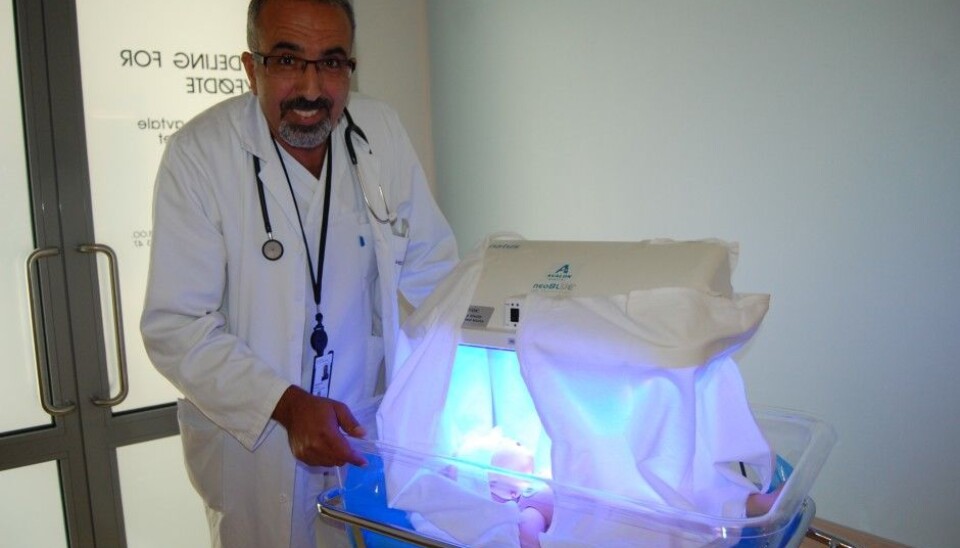
“Light therapy for jaundice—called phototherapy—is the most common treatment given to newborns at Norwegian hospitals. Staff are very aware of the disease,” said Britt Nakstad, lead researcher at Akershus University Hospital’s (Ahus) Child and Adolescent Clinic. Now new research at Ahus has found ways to speed up treatment and increase its effectiveness.
Usually easy to diagnose
Yellow or very red skin is a symptom that allows most cases of jaundice to be diagnosed quickly. Dark skin makes this symptom harder to discern, so then one needs to check whether the whites of the eyes are yellow, or use a special tool to measure the child’s skin for jaundice level.
“Very few children become seriously ill because of undetected jaundice in Norway today. We know of only a single case in the past decade,” says paediatrician Khalaf Mreihil, from the same department at Ahus. But worldwide, jaundice still results in 100 000 deaths annually.
Phototherapy has been around for a while

In 1956, a British nurse chanced to notice that jaundiced infants recovered more quickly when they spent a lot of time in the sun in the hospital courtyard. Wherever their skin had been exposed to light, the normal skin colour returned. Hospitals around the world have been using phototherapy to treat jaundice ever since.
Infant jaundice usually occurs when a baby’s still immature liver is not able to rid the blood of bilirubin. Its yellow pigment gives the skin its yellowish cast. This is the same substance that makes urine yellow.
Bilirubin is toxic to brain cells, and severe jaundice poses the risk of bilirubin passing into the brain and causing damage.
As soon as a jaundiced baby is placed under light, the level of bilirubin in the blood drops.
Shorten the time

Health staff take blood samples of the child during the treatment and remove them from the light when bilirubin levels are no longer dangerous.
“But how quickly the treatment works can vary from place to place, depending on several factors,” says Mreihil.
Until now, not much research has been done on how long the baby should be under the phototherapy lights, or on other conditions that provide optimum results.
Mreihil and his colleagues believe that many newborns spend more time under lights than is strictly necessary.
Finding best practices
Brain damage resulting from jaundice is suspected to be on the rise in the last few years in the USA, according to Lise Lyngsnes Randeberg, Professor of Biomedical Optics at NTNU. “This is because there too, mother and child are sent home so quickly after birth,” she says.
NTNU is developing a mobile app that can detect jaundice, and which will soon allow parents to use their smart phones to check from home whether their child’s skin colour is in the danger zone or not.
For several years, Mreihil has been experimenting with various light sources and the best way for the child to lie in relation to the light. He has measured bilirubin levels in children’s blood at various times during phototherapy sessions. His published research will be part of his PhD thesis, which he hopes to defend next year.
Mreihil has found that bilirubin levels fall after only 15 minutes of treatment. In serious jaundice cases, the best approach is therefore to rapidly get the baby under the lights, even before the blood sample results to come back. He has also identified several other “best practices” to hasten babies’ recovery from jaundice.
Babies have responded most quickly to high light intensity at an ideal distance of no more than 20 cm. Infants should lie on their backs for maximum light exposure, and be unclothed or minimally clothed. “The light doesn’t work through clothing, and we can see this when we look under the diaper where the skin is still yellow. So diapers should be folded back or clipped to expose as much skin as possible,” says Nakstad.
Given these conditions, Mreihil has not found any differences in effectiveness between LED and fluorescent lamps.
Mreihil’s and Nakstad’s study results have been published in Pediatric Research.
Importance of body contact
If paediatric units follow the researchers’ simple recommendations, jaundiced babies will recover more quickly.
But separating a baby from its parents for several hours at a time in the first days of life has disadvantages, too. Long periods of separation compromise the important body contact between the baby and its mother or father.
“In recent years we have become increasingly aware of how essential body contact is for newborns. Prolonged separation from the mother can also affect breastfeeding. Proximity during the first few days is important to get it started,” says Nakstad.
-------------------------------------
Read the Norwegian version of this article at forskning.no
Scientific links
- Khalaf Mreihil, Britt Nakstad et al: Early formation of bilirubin isomers during phototherapy for neonatal jaundice: effects of single vs. double fluorescent lamps vs. photodiodes. Pediatric Research, March 2015. doi:10.1038/pr.2015.61.
- Khalaf Mreihil, Britt Nakstad et al: Early Isomerization of Bilirubin in Phototherapy of Neonatal Jaundice. Pediatric Research, June 2010. doi:10.1203/PDR.0b013e3181dcedc0.