
Fewer people used antibiotics, nasal sprays and cough syrup during the pandemic
This finding is probably due to the coronavirus measures, according to the chief physician at the Norwegian Institute of Public Health.
The Norwegian Institute of Public Health (NIPH) reports that people used fewer antibiotics and cold medicines during the pandemic year 2020.
The figures appear in a new report titled “Medication consumption in Norway 2016–2020”.
Last year 7.4 per cent fewer antibiotics were sold as compared with 2019. The use of prescription cough syrup was halved.
“We see clear changes that are probably a result of the restrictions during the pandemic,” says Hilchen Thode Sommerschild.
Sommerschild is a medical doctor in the Department of Drug Statistics at NIPH.
Annual report
Every year, the Department of Drug Statistics compiles a report that presents the figures for medication use over the previous five years.
The figures are taken from wholesalers who sell to pharmacies, among others. Amounts are measured in defined daily doses, most often stated as grams. The researchers also obtain figures from the prescription database, which indicates how many people have received a prescription for various medicines.
Nasal spray and cough syrup sales down
The researchers noticed that the sales of antibiotics and drugs that are often used for respiratory infections have declined.
“Cosylan is a cough medicine that’s used a lot. It’s a morphine preparation, and sales from last year to this year dropped by half,” says Sommerschild.
Doctors wrote prescriptions for Cosylan for nearly 260 000 people in 2019. In 2020, the number was 130 000. Fewer prescription cough medicines were sold as well, according to figures from the wholesalers.
“There’s been a drop in the use of both prescription and non-prescription cold remedies like nasal sprays, cough suppressants and expectorants,” says Sommerschild.
The researchers noted that over-the-counter sales of ibuprofen and acetaminophen (or paracetamol) skyrocketed in March 2020. Most likely people were hoarding them at the outset of the pandemic, and later sales normalized.
Clear decline
All told, fewer antibiotics were used.
“We looked at various types of antibiotics to see if there were differences,” says Sommerschild, and she found that there were.
“The amount of antibiotics used mainly for respiratory infections showed a steep decline.”
Antibiotics used for urinary tract infections, wounds and skin infections didn’t see reduced sales in the same way.
Sommerschild says this difference is likely due to the coronavirus measures.
“Respiratory tract infections are contagious and thus greatly affected by social distancing, in contrast to UTIs, for example.”
“But there could be one more factor here. The threshold for consulting a doctor or the health service has probably also been higher,” says Sommerschild.
Biggest change in the littlest ones
Among young children between the ages of 0 and 4, 40 per cent fewer took antibiotics in 2020 than in the year before.
The decline among the elderly was not as noticeable, but there were still 7 per cent fewer people over the age of 75 who took antibiotics in 2020.
The graph below shows the percentage of the population that took antibiotics in different age groups. The pale lines show the percentage of men and women who took antibiotics in 2019, and the darker lines show the figures for 2020.
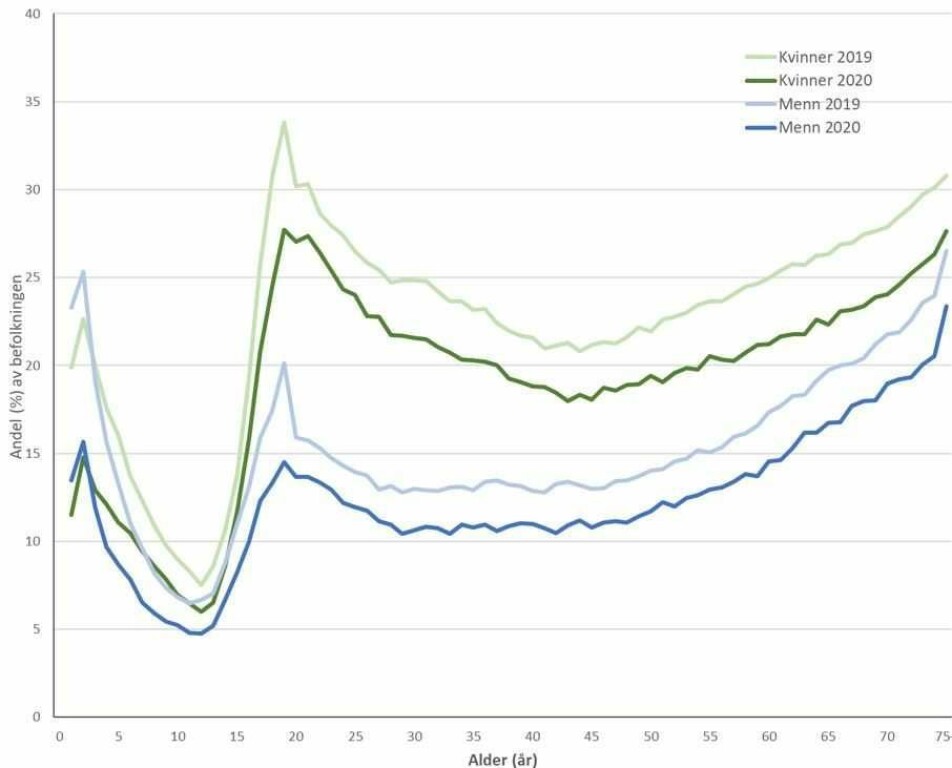
“In 2019, you see a sharp peak that corresponds to 19-year-olds. That peak is almost non-existent in 2020,” says Sommerschild.
This probably has to do with the high school senior “russ” celebrations, culminating at the 17 May parade.
“The 19-year-olds are out partying a lot, and then they get colds. After 17 May, they go on antibiotics so they’ll be healthy by exam time. Researchers have studied this before by looking at how cold medicine use is distributed over the relevant months,” Sommerschild says.
In 2020, there wasn’t as much senior partying as the year before and the peak flattened out.
No big difference in antidepressant use
Sommerschild is not really surprised that antibiotic use fell so much during the pandemic.
“We expected to see less use of medication for infectious respiratory infections,” she says.
Sommerschild also finds it interesting to look at some other medicine groups where one would expect change.
“There’s been a lot of talk about isolation and loneliness during the pandemic. So we might think that the use of medication for depression, anxiety, restlessness and pain would increase. When we look at groups of these drugs and their use across the entire population, we don’t see any striking change. But these are very rough numbers,” she says.
A lot can hide under the surface, and she notes that researchers have numerous opportunities to dive further into the material.
If we look more closely at gender, age groups, patient groups, times of the year, the individual drugs and so on, a different picture may emerge.
Special flu season
The decline in the use of antibiotics and common cold medicine indicates that fewer people were suffering from respiratory infections last year.
This finding is in line with the number of confirmed flu cases last season.
“The incidence of influenza this season has been at an all-time low,” says Olav Hungnes.
He is a researcher at the Norwegian Institute of Public Health and heads the National Influenza Centre.
In total, only 11 cases of influenza were detected, according to NIPH’s last weekly report for the 2020-2021 flu season.
Reference:
Hilchen Thode Sommerschild et al.: “Drug consumption in Norway 2016–2020”, NIPH, June 2021.
Translated by Ingrid P. Nuse.
Read the Norwegian version of this article on forskning.no.
































