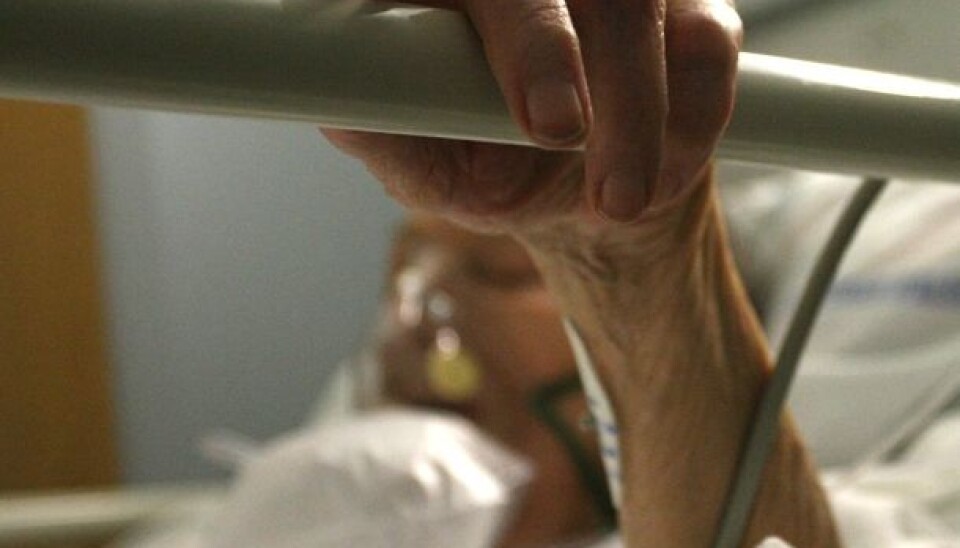
Norwegians suffer more painful deaths than necessary
Norwegian health personnel don’t administer enough pain relief to the dying. New research shows that this is partly due to fears of being accused of euthanasia.
Denne artikkelen er over ti år gammel og kan inneholde utdatert informasjon.
The only sure thing at birth is that some day will be our last.
Last year 42,000 Norwegians died. This was 600 more than in 2011. The increase is linked to demographics, because the percentage of old people in this country of five million is on the rise.
Eight out of ten die in hospitals or nursing homes, according to the nursing website sykepleien.no.
Far too many of them suffer severe pain at the end of their lives. This is suffering that could be averted, according to researcher Simen A. Steindal of Diakonhjemmet University College.
Final three days

Steindal has perused the records of 220 patients who died in hospitals and focused on the last three days of their lives.
Half were cancer patients, while the other 110 died of other diseases.
The researcher concludes that one in three of these terminal patients received insufficient pain relief.
Several of the records noted that painkillers were given but that the patients still complained of pain.
“Health personnel may give insufficient doses out of fear of fatal side-effects and being accused of practicing euthanasia,” Steindal says.
“Opioids such as morphine compounds are the most common pain treatment for cancer patients, but they can also cause a patient to stop breathing,” he explains.
So the doses are often increased incrementally − and in some cases too slowly.
The researcher adds that the next of kin or the patients sometimes decline pain-relief treatment, or request lower doses than are called for, because the treatment can pose a risk of shortening a life.
Steindal’s research also showed it can be hard to determine the actual reasons why health care personnel don't provide enough pain relief.
He also found that health personnel don't do a good enough job recording the pain suffered by patients.
Little focus on pain in colleges
One problem is that information about pain intensity is not recorded in a patient's records when the patient has a disease other than cancer.
“This could be because health personnel know that cancer is associated with pain, but that they may not be as aware of this problem with other illnesses,” says Steindal.
According to the Norwegian Medical Association, 90 percent of cancer patients suffer pain in their final days.
All patients have a right to a satisfactory diagnosis and treatment of pain, according to Norway’s Health Personnel Act. And evaluations and treatment of pain are supposed to be recorded in patient records.
The Norwegian Medical Association writes in its guidelines for palliative treatment that the basic Norwegian medical education puts little emphasis on pain and pain relief, and the subject is being reduced rather than increased:
Educational provisions should be generally expanded. Norway does not offer any special field or sub-special field in palliative treatment, whereas several other countries offer this discipline as is a special field (USA) or sub-special field (Sweden, Finland and other countries in Europe). [editor’s translation]
Below WHO’s expectations
Steindal says that the World Health Organization has concluded that it’s possible to provide acceptable pain relief to 97 percent of all patients if the clinical guidelines for palliative treatment are followed.
This means three percent still cannot be helped. Steindal says it is problematic that ten percent of the patients in his study received inadequate help for their pain.
The researcher also thinks a lot of cases go unrecorded.
“I’ve only read the medical charts, and it’s likely that the figure would have been even higher if I’d had the opportunity to ask the patients themselves.”
He adds that health personnel can misinterpret uneasiness as pain among patients who are unable to communicate.
On the other hand, he refers to research showing that health personnel often underestimate pain in older patients.
So pain is both under-reported and undertreated.
Steindal thinks better documentation of patients’ pain and how health personnel choose to treat this pain are necessary:
“Then everyone who has something to do with the patient has access to good information in the record and pain issues will be given more focus, also for patients with other diseases than cancer.”
Quality of life
Georg Bollig is a board member of the Norwegian Palliative Association (NPF), chief physician in a German hospital palliative team and a researcher at the University of Bergen.
Palliative treatment is given to patients with incurable diseases in the terminal phase. The treatment consists of relieving pain or other symptoms to improve the quality of what little life the patient has left.
Bollig confirms that families and patients themselves sometimes think that too little pain relief given as death closes in.
But he won’t speculate on how often this occurs.
“I don’t think palliative treatment in Norway is poor, but we could say that it can be improved in the Norwegian health system,” says Bollig.
“This need for improvement is a problem in most countries. Part of the problem is how pain treatment is documented,” he adds.
He says that NPF wants to change attitudes toward care in the terminal stage, both among medical staff and the general public.
“We should focus more on life quality than life prolongation.”
Reference:
Steindal , Simen Alexander: Symptoms, clinical signs, and treatment of hospitalised patients in the last three days of life - healthcare workers’ documentation, June 7 2013.
----------------------------
Read the Norwegian version of this article at forskning.no
Translated by: Glenn Ostling